UnitedHealth: Chronic conditions becoming more prevalent as disparities emerge
In 2022, more than 29 million adults reported having three or more chronic conditions, and disparities emerged among many demographic groups.

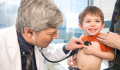
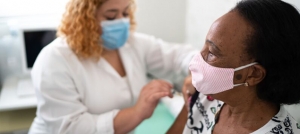
Photo: SDI Productions/Getty Images
Multiple chronic conditions, ranging from diabetes to depression, are becoming more common, according to the United Health Foundation, the philanthropic arm of UnitedHealth Group. Many chronic conditions are at the highest levels ever recorded in the annual report.
, released in partnership with the American Public Health Association, examines 87 measures of health from 28 distinct data sources to present a comprehensive overview of the health and wellbeing of the nation.
In 2022, more than 29 million adults reported having three or more chronic conditions, and disparities emerged among demographic groups, such as the management of diabetes, asthma and cardiovascular diseases among certain racial/ethnic groups.��
WHAT'S THE IMPACT?
Eight chronic conditions – arthritis, depression, diabetes, asthma, cancer, cardiovascular diseases (CVDs), chronic obstructive pulmonary disease (COPD) and chronic kidney disease (CKD) – reached their highest levels since America's Health Rankings began tracking these measures.��
Notably, between 2021 and 2022, depression prevalence surged to 21.7%, affecting nearly 54.2 million adults. Diabetes prevalence also increased to 11.5%, impacting nearly 31.9 million adults, while asthma prevalence rose to 10.4%, affecting nearly 26 million adults.
Numerous disparities were uncovered across nearly every measured demographic group. For example, looking at disability status, COPD was 7.7 times higher (26.3% vs. 3.4%), CKD was 6.5 times higher (13.7% vs. 2.1%) and asthma was 3.2 times higher (23.4% vs. 7.4%) among adults who reported self-care difficulty than those without a disability.
Race was also a factor, with COPD��7.1 times higher among American Indian/ Alaska Native (10.6%) than Asian (1.5%) adults, and cancer 3.9 times higher among white (10.8%) than Asian (2.8%) adults.
Others fell along geographic lines: Depression was 2.3 times higher in Tennessee (29.2%) than Hawaii (12.5%), while diabetes was 2.1 times higher in West Virginia (17.4%) than Colorado (8.1%). Veteran status also mattered – CVDs were 2.1 times higher (17.6% vs. 8.3%) and cancer was 1.8 times higher (13.5% vs. 7.6%) among adults who have served in the U.S. armed forces than those who hadn't��served.
Other notable disparities pertained to sexual orientation. Depression was 2.4 times higher (45.4% vs. 19.2%)��and asthma was 1.6 times higher (15.2% vs. 9.7%)��among adults who identified as LGBQ+ than straight adults,��and cancer was 1.7 times higher among adults who identified as straight (8.7%) than LGBQ+ adults (5%).
THE LARGER TREND
The report also found that the number of mental health providers – including psychiatrists, psychologists, licensed clinical social workers, counselors, marriage and family therapists – increased 7% between 2022 and 2023.��
However, the demand for mental health services may have also increased in the past several years, as demonstrated by an 8% increase in frequent mental distress – the percentage of adults who reported their mental health was not good 14 or more days in the past 30 days – from 14.7% to 15.9% between 2021 and 2022.
Meanwhile, the number of primary care providers decreased 13% over that time. This resulted in a nationwide decline of over 107,000 providers. There were striking disparities in the number of primary care providers between states: The number of providers per 100,000 people was 1.8 times higher in Massachusetts than in California.
��
Twitter: @JELagasse
Email the writer:��Jeff.Lagasse@himssmedia.com