Moody's upgrades healthcare outlook from negative to stable for 2024
The bottom line is hospitals' operating cash flows and margins will improve and revenue growth will slightly top expenses.

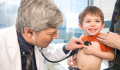
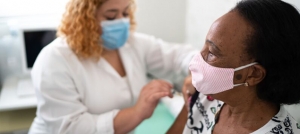
Photo: sturti/Getty Images
Moody's Investors Service has revised its 2024 outlook for the not-for-profit and public healthcare sector to stable from negative, driven in large part by a decrease in labor costs.
While hospitals will continue to grapple with high expenses because of a shortage of skilled labor, particularly nurses, Moody's predicts that the growth in expenses will slow as hospitals make greater efforts to recruit and retain full-time staff, partly through providing expanded benefit packages. This will reduce reliance on expensive contract labor.
Still, with union activity on the rise nationwide, contract negotiations could become more contentious, resulting in work stoppages and hefty wage increases, Moody's said.听
WHY THIS MATTERS
Hospitals, physician practices and other providers have been grappling with labor shortages and higher expenses due to hiring travel nurses to fill the gap.
Alternatives to expensive contract labor are expected to help revenue, as is听a modest rebound in patient volumes and higher reimbursement rates.
These factors signal a financial recovery that will increasingly take hold in 2024, marked by an uptick in cash flow margins, Moody's said.听
Though reimbursement rate increases from insurers will rise in the mid-single-digit percentage-range on average in 2024, they will not fully compensate for the recent expense increases due to inflation, Moody's said.听
In some cases, higher reimbursement rates negotiated with insurers and modest patient volume increases will drive median operating revenue growth in the 4%-6% range in 2024, Moody's predicts.
Growth in operating cash flow margins will allow many hospitals to make needed investments in facilities and programs and maintain liquidity听
Increased state financial backing and Federal Emergency Management Agency (FEMA) funds will aid some healthcare providers' financial turnaround.
Risks include government policies such as Medicare reimbursement levels that are not keeping up with inflation and the end of a pandemic-era provision preventing states from Medicaid disenrollment, which could lead to higher uncompensated coverage.
The 340B program, which allows some hospitals to purchase drugs at a discount, will continue to face scrutiny, with limits on usage of contract pharmacies possibly hurting eligible hospitals through operating income losses, Moody's said. However, some health systems may benefit from a one-time payout from prior-year 340B reimbursement true-ups in 2024.
The rate of consolidation among health systems may slow due to increased scrutiny of mergers by federal and state governments, potentially depriving distressed systems of exit strategies and slowing the growth of larger systems active in the M&A space, the report said.听
Additionally, potential requirements for nurse-to-patient staff ratios could increase labor costs and exacerbate staffing shortages, especially at post-acute-care facilities.
The bottom line is hospitals' operating cash flows and margins will improve, and revenue growth will slightly top expense growth, but this will call for strict expense management to maintain a path to recovery.
THE LARGER TREND
Moody's said the outlook could move to positive if the median operating cash flow margin is above 8%, likely driven by significantly slower expense growth and better reimbursement prospects.听
A substantial rise in labor or supply costs听or a disruption in volume recovery听could again lead to a negative outlook.
Insurers' denial of claims will impact providers. Revenue-cycle management will be critical as costs collecting patient payments remain high, partly because of insurers aggressively denying coverage and requiring extensive pre-authorization, Moody's said.
Revenue growth will be constrained by denied reimbursement claims and payment delays, while demand for extensive documentation by private payers is expected to increase hospitals' costs and time needed for revenue collection.
Growth in managed care plans such as Medicare Advantage, where insurers have a greater denial incentive than plans in which they simply administer payments with no insurance risk, will likely lead to more denials.听
In turn, Moody's said it anticipates a rise in lawsuits by hospitals for underpayment and contract violations, leading to more contentious contract renegotiations with insurers and terminations in relationships. High-profile lawsuits and terminations could spur legislative intervention that alters the negotiating landscape.
Twitter: @SusanJMorse
Email the writer: SMorse@himss.org