Mental health inequities resulting in billions in expenses, Deloitte finds
These costs could total about $478 billion through the rest of the year and balloon up to $1.3 trillion by 2040.

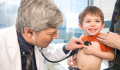
Photo: Basak Gurbuz Derman/Getty Images
Mental health inequities may not only harm individuals but also hinder economic prosperity.
A new Deloitte projects mental health inequities could total about $478 billion in avoidable costs throughout the rest of this year.
Left unchecked, the numbers suggest this could balloon up to $1.3 trillion by 2040. That's equivalent to about $42,000 per person living in the U.S.
Premature death was one of the major drivers of these expenses. Analysts said avoidable costs linked to premature deaths topped $292 billion in 2022 and project that if the current cost trajectory remains unchanged, the annual cost of premature deaths in 2040 could reach almost $912 billion.��
The other major mental health-related factor ramping up expenses is productivity loss, which is projected to account for about $116 billion in avoidable costs this year. The research corroborated previous findings showing a link between mental health conditions and productivity losses, with depression in particular serving as a major contributor to workplace absenteeism. Affected individuals take more sick days compared to their non-depressed counterparts, the report said.
Presenteeism – the phenomenon of being present at work but not fully functioning due to mental health issues – is another significant factor reducing productivity. Additionally, mental illness can lead to disability claims, resulting in prolonged periods of reduced or lost productivity and additional insurance costs.
WHAT'S THE IMPACT?
Certain demographics are disproportionately affected by these trends, in particular some racial/ethnic groups, members of the LGBTQIA+ community, low-income individuals, people living with disabilities and those involved in the justice system, including parolees and incarcerated individuals.
Although the white population shows the highest prevalence of mental health diagnoses, it is the nonwhite population that tends to bear more of the cost associated with mental health struggles. Authors attribute this to the long-standing structural racism and the legacy of policies that disadvantage certain populations, as well as social and economic conditions.
In general, higher prevalence of mental health conditions and higher prevalence of other chronic conditions are correlated. Lower-income populations with mental health challenges have a higher prevalence of other chronic conditions, the report found. The estimates are likely low due to cultural stigma and lack of access to care.
Groups with mental health challenges account for more work days missed and have a higher rate of unemployment than those without such challenges. For those with mental health conditions, a higher prevalence of other chronic conditions, more days missed from work and higher unemployment are seen across all age groups.
According to the report, decreasing health inequities could lower health-plan and system costs associated with the poor health outcomes that lead to more emergency room visits, longer hospital stays and unnecessary hospitalizations. This in turn could generate value for the businesses that pay for healthcare, as well as state and federal agencies.
Improving health outcomes could also improve quality ratings of both plans and providers, making them eligible for higher payments from Medicare and other value-based care programs designed to reward quality, authors said.
Although equity-centered initiatives will require additional targeted spending, the data indicates that achieving mental health equity can avoid a higher cost burden in the long run.
These initiatives may include academic research; establishing integrated care models; employers providing more mental health and wellbeing resources; and local governments distributing providers and other resources to the places where they are most needed and least found, such as neighborhoods characterized by a high mental health need.
THE LARGER TREND
A 2023 KFF study found the ongoing mental health crisis in the U.S. is also disproportionately straining Medicaid, in part because behavioral health services cost the federal program more than they did other payers.
In addition, workforce challenges contribute to barriers in access to care and nearly half the U.S. population – 47%, or 158 million people – live in a mental health workforce-shortage area. Workforce challenges are widespread, and go beyond Medicaid, but shortages may be exacerbated in Medicaid, according to the analysis.
��
Jeff Lagasse��is��editor of Healthcare Finance��News.
Email:��jlagasse@himss.org
Healthcare Finance��News is a��HIMSS��Media publication.